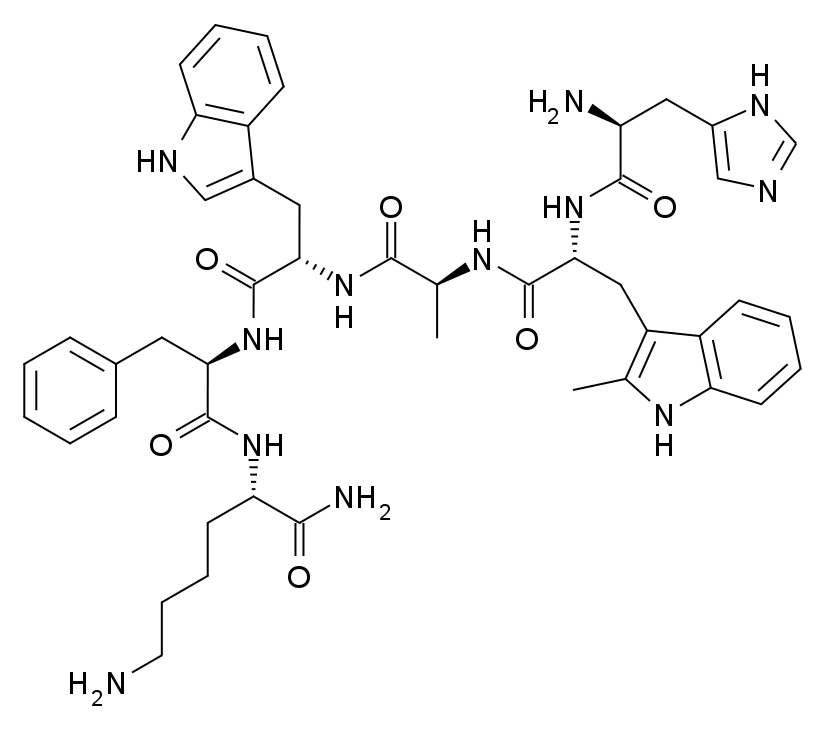
Hexarelin has been studied in a foundational pharmacology paper (Deghenghi 1994), Phase I PK/PD work on bioavailability and hormone profile (Imbimbo 1994; Ghigo 1994; Massoud 1996), one longitudinal paediatric pharmacology study (Klinger 1996), three human cardiovascular studies (Bisi 1999; Imazio 2002; Broglio 2002), the canonical CD36 mechanistic paper (Bodart 2002), a contemporary review (Mao 2014), and a preclinical post-MI study (McDonald 2018). All findings are reported as investigational and for research use only.
Acute GH-releasing pharmacology in healthy adults — multiple administration routes (Ghigo 1994)
Phase I Studies report, in an open-label PK/PD study in N=12 healthy young male volunteers, that GH release after 1 µg·kg⁻¹ i.v. hexarelin was approximately twice that produced by 1 µg·kg⁻¹ GHRH. Bioavailability: subcutaneous 77.0 ± 10.5 %, intranasal 4.8 ± 0.9 %, oral 0.3 ± 0.1 %; plasma half-life ≈ 55 min.
— Ghigo et al., J Clin Endocrinol Metab 1994;78(3):693–698 (PMID 8126144)
Dose-response of GH, prolactin, and cortisol (Massoud 1996)
Phase I Studies report, in a dose-response pharmacological study in healthy adult males (hexarelin 0–1.0 µg·kg⁻¹ i.v.), maximum GH release plateauing at ~140 mU·L⁻¹ (ED₅₀ ≈ 0.48 µg·kg⁻¹), prolactin rising up to 180 % above baseline (ED₅₀ ≈ 0.39 µg·kg⁻¹), and cortisol increasing ~40 % at 0.5 µg·kg⁻¹ — quantitatively higher than ipamorelin. Combination of low-dose hexarelin (0.125 µg·kg⁻¹) with GHRH produced massive GH release (~115 mU·L⁻¹) with minimal cortisol elevation.
— Massoud et al., J Clin Endocrinol Metab 1996;81(12):4338–4341 (PMID 8954038)
Acute cardiac inotropic effect in healthy humans (Bisi 1999)
Phase I Studies report, in a cross-over hormonal/cardiovascular study in N=7 healthy male volunteers using radionuclide angiocardiography, an LVEF increase from 64.0 ± 1.5 % to 70.7 ± 3.0 % (P < 0.03) after i.v. hexarelin, peaking at 30 min and persisting ~60 min, WITHOUT significant change in mean blood pressure or heart rate. Recombinant human GH (rhGH) produced NO comparable inotropic change despite similar GH elevation — supporting a GH-independent myocardial action (later attributed to CD36).
— Bisi et al., J Endocrinol Invest 1999;22(4):266–272 (PMID 10342360)
CD36 as the molecular cardiac receptor — knockout pharmacology (Bodart 2002)
preclinical Studies report, in a receptor-identification experiment in isolated rat heart preparations, that hexarelin produced a dose-dependent rise in coronary perfusion pressure in wild-type hearts; the response was ABOLISHED in CD36-deficient hearts despite preserved GHSR-1a expression — establishing CD36 as the cardiac receptor for hexarelin and other GHRPs.
— Bodart et al., Circ Res 2002;90(8):844–849 (PMID 11988484)
Cardiac performance in coronary-artery-disease patients (Broglio 2002)
Phase II Studies report, in an open-label intra-operative pharmacological study during coronary artery bypass surgery in N=24 male CAD patients (mean age 59.5 yr), a prompt rise in LVEF, cardiac index, and cardiac output (all P < 0.001) within 10 min of i.v. hexarelin, lasting up to 90 min, WITHOUT changes in left-ventricular end-diastolic volume or systemic vascular resistance. Neither rhGH nor GHRH reproduced these haemodynamic improvements — consistent with a non-GH cardiac mechanism.
— Broglio et al., Eur J Pharmacol 2002;448(2-3):193–200 (PMID 12144941)
Cardiotropic activity in left-ventricular dysfunction (Imazio 2002)
Phase II Studies report, in a comparative open-label cardiotropic study in N=13 patients (8 dilated + 5 ischaemic cardiomyopathy) given single-dose i.v. hexarelin, that LVEF rose in ischaemic-cardiomyopathy patients but NOT in dilated-cardiomyopathy patients — despite a comparable hexarelin-induced GH rise in both groups. The inotropic effect appears to require viable myocardium capable of responding to direct CD36/GHSR-mediated cardiotropic signalling.
— Imazio et al., Eur J Heart Fail 2002;4(2):185–191 (PMID 11959048)
GHSR-1a desensitisation under long-term dosing (Klinger 1996)
observational Studies report, in an open-label longitudinal pharmacology study in N=7 prepubertal short children (mean age 7.6 yr) on intranasal hexarelin 60 µg·kg⁻¹ three times daily for 6–10 months, that the peak GH dropped from 70.6 mU·L⁻¹ at baseline to 34.1 mU·L⁻¹ after 7 days (~50 % attenuation), then plateaued — confirming receptor desensitisation. Despite biochemical tolerance, growth velocity rose from 5.3 ± 0.9 cm·yr⁻¹ pre-treatment to 7.4 ± 1.6 cm·yr⁻¹ at 6–10 months. Follow-on studies show ~50–75 % AUC-GH attenuation over 4–16 weeks of daily dosing, partially reversible after washout — wellness-market claims of sustained "anti-aging" elevation are NOT supported by this evidence.
— Klinger et al., Eur J Endocrinol 1996;134(6):716–719 (PMID 8766941)